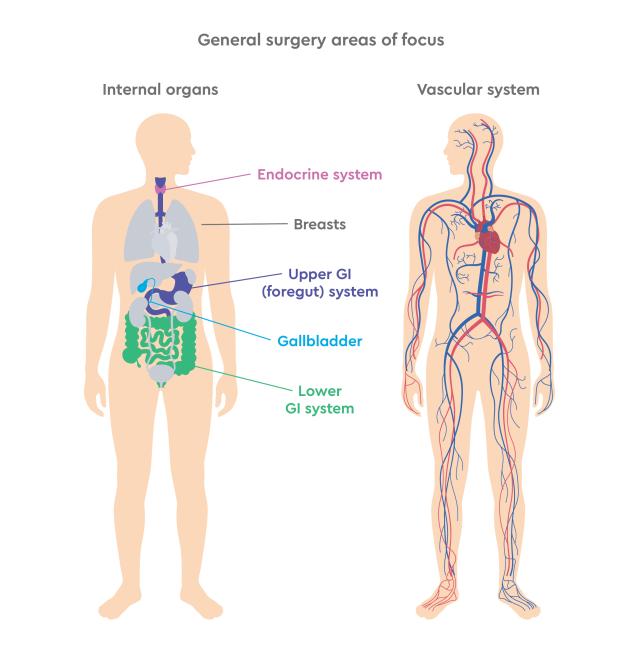
Gastrointestinal cancers
Genitourinary cancers
Gynecological cancers
Cancers & Diseases
We’re here to get the best possible life outcomes for every cancer patient. We do that by combining the right clinical teams with innovative and effective treatments.
Medical specialties
Surgical specialties
Treatments & Services
By working with leading experts across a range of specialties, we provide many of the latest treatments and services from around the world that are proven to be effective.
About us
A cancer and multispecialty network in Florida providing care for more than 90,000 patients annually. We offer community-based cancer care and other services at convenient locations.

Patient Resources
Common questions
Patient Support
We don't treat cancer, we treat the patient. We believe care should be focused on you, the individual, not your condition.